What's really the deal with toxoplasma gondii and human behavior?
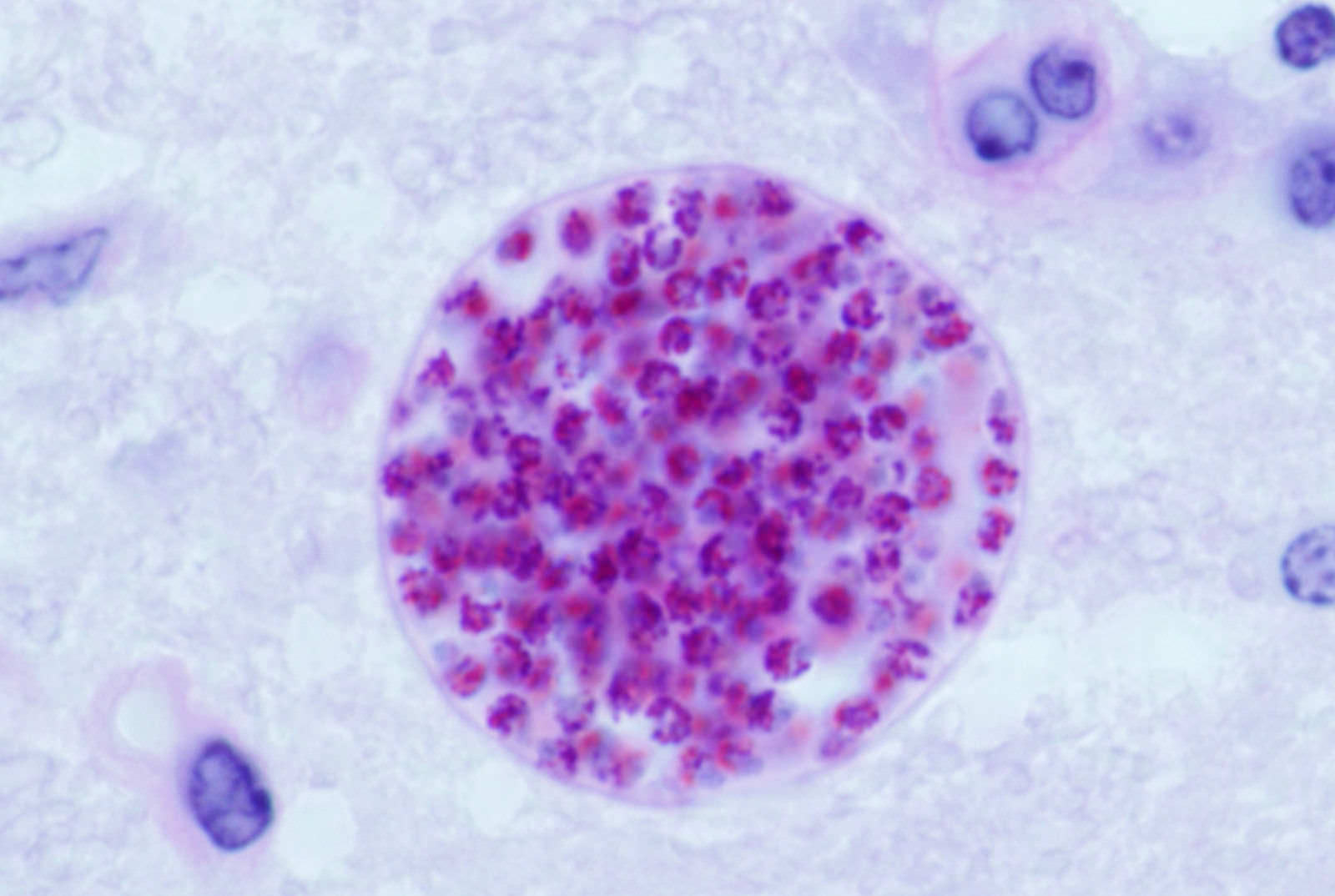
T. gondii cyst in a mouse brain.
For a simple protozoan, Toxoplasma gondii has experienced something of a meteoric rise in popularity over the past several years. Actually, to be fair T. gondii has garnered quite a bit of interest since the 1930s, when it was discovered the parasite could be transmitted from a mother to a fetus in the womb, sometimes resulting in severe congenital disorders. Curiosity about T. gondii grew significantly in the early 2000s, however, when it was found that T. gondii infection in mice and rats might influence the behavior of the rodents so as to make them less afraid of cats.
Recently, interest in T. gondii has been especially focused on the hypothesis that the microorganism might also be able to influence human behavior. Indeed, this idea has become a popular topic of discussion even outside the sphere of research. This notoriety, however, has led to a spectrum of opinions that range from the suggestion T. gondii is responsible for a variety of psychiatric symptoms to the viewpoint that there is no sound evidence at all to indicate such a thing. Is one of these perspectives more accurate than the other?
T. gondii and rodent behavior
Effects of T. gondii infection on rodent behavior have been recognized since the late 1970s when it was observed that infected mice displayed impaired performance on memory tasks. Various other studies over the next couple of decades noted effects on behavior and cognition in rodents, but widespread interest in the behavioral effects of T. gondii infection was triggered by the publication of a study that suggested T. gondii-infected rats exhibit a diminished aversion to cat urine---and that some infected rats may even display an attraction to it. This effect was eventually seen in mice as well.
This finding was compelling when placed in the context of something called the parasite manipulation hypothesis, which states that some parasites have evolved mechanisms to influence their hosts so as to promote the parasite's transmission. This hypothesis was thought to make sense when used to describe T. gondii because T. gondii is only capable of reproducing within the intestines of cats; felines thus play an essential role in the life cycle of the parasite. After reproduction, however, several million oocysts (sort of a protozoan parasite version of an embryo) are expelled from the feline intestines in the feces. Unfortunately for these oocysts, this causes them to be forced out of their preferred feline intestinal environment, seemingly without a clear path of return. That is where rodents come in.
Many animals who are exposed to the feces of an infected cat (e.g. through contaminated food or drinking water) can become infected with T. gondii. Rodent infection, however, might be especially useful to T. gondii due to the role of cats as natural predators of rodents. Some have suggested that the ability of T. gondii to reduce rodent fear of cat urine gives T. gondii a method by which to find its way back to its preferred environment. By making rodents less cautious around cat urine, which previously had acted as a distinct threat-identifying odorant, rodents may put themselves in harm's way and be more likely to be eaten by cats. If they are, T. gondii ends up right where it needs to be to reproduce and continue its life cycle.
Neuronal mechanisms for T. gondii action
In order to manipulate the behavior of rodents it would seem necessary for T. gondii to have a means by which it could influence neurobiology; of course, such a mechanism would also be necessary for the manipulation of human behavior. What exactly this mechanism might be is still under investigation, but one thing that's certain is that T. gondii does have a way of making it to the brain of its host, whether that host be a human or a rodent. Indeed, T. gondii invasion of the central nervous system is associated with the most severe complications of T. gondii infection in humans, and by some estimates T. gondii may cross the blood-brain barrier and enter the brain as quickly as 7 days after infection occurs.
Once T. gondii is in the brain, it can infect neurons directly. What happens as a result is still uncertain, but several hypotheses have been proposed to explain the ways T. gondii infection can disrupt neuronal function. One hypothesis is that T. gondii infection of neurons can alter dopamine metabolism to increase dopamine synthesis and release. Another hypothesis contends that T. gondii infection can influence calcium signaling in such a way as to make neurons either hypo- or hyper-responsive. A complete model of T. gondii's effects on neurons has not yet been elucidated, however, so the true mechanism may involve these processes or something different altogether.
When T. gondii enters the brain, it also infects glial cells like microglia and astrocytes; activation of these cells is associated with the production of a general inflammatory response in the brain. This neuroinflammation may have a variety of effects on neurobiology, including influences on neurotransmitter metabolism, changes in neurotransmitter receptor levels, and effects on synaptic morphology or connectivity. Thus, the repercussions of inflammation caused by T. gondii infection may also be extensive enough to modify the behavior of the host.
While there is much to still be understood about the way or ways in which T. gondii can affect host behavior, there are at least plausible mechanisms identified by which such an effect might occur in mammalian hosts (including humans). And, when we are investigating the potential of an exposure like T. gondii infection to cause an effect on a host, biological plausibility can support the argument that the potential exists. In other words, if there were no plausible biological mechanism by which T. gondii could influence behavior, then we would be less confident it is actually affecting behavior (even when studies like those discussed below find some correlation between infection and behavioral changes). Just because there is a biologically plausible manner by which T. gondii can influence behavior, however, doesn't mean it actually does. To be confident about the relationship between T. gondii and human behavior we also need some strong evidence showing a relationship between infection and behavioral changes in human populations.
T. gondii and human behavior
The relationship between T. gondii infection and human behavior has been a subject of research for many years, and studies of the prevalence of T. gondii infection in psychiatric patients date back to the middle of the 20th century. However, the suggestion that T. gondii may be manipulating rodent behavior led to a resurgence of interest in T. gondii 's potential to affect people. Along with that increase in research-related interest came heightened interest from the popular press, which caused the potential influence of T. gondii on psychiatric symptoms to become a trendy---but often sensationalized---topic.
Regardless, legitimate research into this topic continues to be conducted; by now researchers have explored the potential association between T. gondii infection in humans and a wide range of behavioral and psychiatric outcomes. And, a number of studies have detected correlations between the presence of T. gondiii antibodies and behavioral or psychiatric abnormalities. For example, one study found T. gondii infection to be associated with increased aggression in women and increased impulsivity in younger men. Another study detected a correlation between homicide rates and rates of T. gondii infection in the population. Other findings include links to suicide rates and even traffic accidents (hypothetically due to the effect of the parasite on characteristics like reaction time).
By far, though, it seems the most frequently investigated relationship between T. gondii infection and psychiatric abnormalities is the association between T. gondii and schizophrenia. Over 40 studies examining the relationship between T. gondii infection and schizophrenia or psychotic symptoms have been published since the 1950s. In 2012, a group of researchers synthesized data from 38 of these studies to determine if there was a consistent association between T. gondii infection and schizophrenia. The results of this analysis suggested that, across all of the studies included, individuals who had been diagnosed with schizophrenia were about 2.73 times more likely to also be infected with T. gondii. In terms of how this increase in risk stacks up against other known risk factors for schizophrenia, it is similar in magnitude to the increase in risk of schizophrenia seen in those who grow up in an urban environment or in those who have a father who is age 55 or older at birth, but significantly lower than the increased risk imparted by having another immediate family member with schizophrenia.
Based on this information along with the biological plausibility of T. gondii's mechanism for affecting brain activity, it may sound to you like there is something to the idea that T. gondii infection can lead to psychiatric disorders (or schizophrenia in particular). However, there are some reasons to take all of these T. gondii findings regarding human behavior with a grain of salt. One is that the studies conducted up to this point generally have followed this methodology: get a sample of individuals, test them for antibodies to T. gondii (which would indicate an infection if present), and look for correlations between the presence of antibodies and schizophrenia (or some other psychiatric outcome).
While a study like this can be informative, it leaves many questions unanswered. For example, even if this type of study finds a link between T. gondii and schizophrenia, because data was only collected at one point in time it is impossible to tell if the T. gondii infection preceded (and thus caused) schizophrenia. This allows for a number of other possible explanations for the relationship between infection and schizophrenia. For example, there is a possibility that the correlation between T. gondii infection and schizophrenia exists because infection becomes more likely after the onset of schizophrenia. What if, for instance, the onset of schizophrenia is associated with behavioral changes (e.g. eating and hygiene changes specifically) that increase exposure to sources of T. gondii contamination?
Alternatively, what if some common variable increases the risk of both T. gondii infection and schizophrenia? For example, what if something about one's neurobiology makes one more likely to own a cat (and thus be exposed to T. gondii through exposure to cat feces) and also predisposes one to schizophrenia? Or, what if T. gondii doesn't increase the risk of schizophrenia, but some other microorganism passed from a cat to a human does? In that case, owning a cat would make someone more likely to be infected with T. gondii and more likely to develop schizophrenia, but not due to a direct link between T. gondii and schizophrenia. Indeed, one study found no significant link between T. gondii infection and schizophrenia, but did find a significant association between having close contact with cats and schizophrenia. In the end, the problem is that observational studies that rely on data collected at only one point in time allow for too many other possibilities to let us have any confidence that there is a causal relationship between the variables we are interested in. Hence these studies can detect correlation, but not causation.
With this in mind, one way to get closer to some answers to these questions about T. gondii and psychiatric symptoms is to conduct more studies using longitudinal designs. A longitudinal study design, for example, would begin with a sample of overtly healthy people---some people who were infected with T. gondii and some who were not; these individuals would then be followed up with over a period of years to see if those with T. gondii infection were more likely to subsequently develop psychiatric disorders. This approach can provide more convincing evidence of a causal relationship, in part because it can provide insight into whether T. gondii infection precedes the onset of the symptoms (since at the start of the study the symptoms were not present).
Because of the paucity of studies that have the ability to detect causal links between T. gondii and human psychiatry, there are researchers who argue that some are inferring a causal relationship when the evidence for that causal relationship doesn't exist. For example, a recent study looked at the association between T. gondii infection and a number of psychiatric measures ranging from IQ to schizophrenia diagnosis. The authors found no link between T. gondii infection and shizophrenia or most other psychiatric measures, and in the concluding paragraphs they suggest that "earlier reports of links between T. gondii infection and behavioral impairments are exaggerated," due in part to the intrigue both researchers and the public have with the idea of T. gondii being able to manipulate human behavior. Interestingly, the study in question did actually detect a link between T. gondii infection and recent suicide attempts, suggesting that perhaps the idea the pathogen is influencing behavior is not entirely unreasonable.
Regardless, although there are some titillating findings concerning T. gondii infection and psychiatric disorders, at this point it is not a relationship we can be very confident in. This is not to say that there is no ground for the hypothesis to stand on, but instead that more research is needed before we can decide if the microorganism is really having some influence on human behavior. Despite the lack of strong evidence, however, there is likely a reason that infectious origins of psychiatric disorders has been such a popular topic in recent years. It's mind-boggling for most of us to imagine that this complex, highly-evolved organ we call the human brain can be manipulated and turned dysfunctional by organisms that have a diameter on the scale of micrometers. It creates for us a strangely wonderful sense of impotence that causes us to step back and reassess the position of superiority we generally give ourselves over other organisms. And that reminder of our own helplessness to control some aspects of the natural world can be both frightening and fascinating at the same time. Thus, the idea is inherently captivating, and it is likely to continue to attract speculation and exaggeration until we come to a more definite conclusion on its accuracy.
Parlog A, Schlüter D, & Dunay IR (2015). Toxoplasma gondii-induced neuronal alterations. Parasite immunology, 37 (3), 159-70 PMID: 25376390