Know Your Brain: Blood-Brain Barrier
Where is the blood-brain barrier?
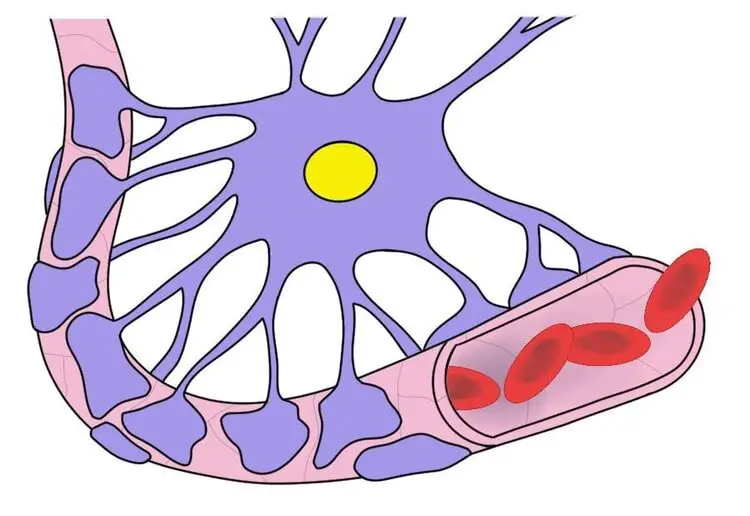
The blood-brain barrier surrounds most of the blood vessels in the brain. It is a structure that is formed primarily due to the establishment of tight junctions between endothelial cells (i.e., cells that line the walls of blood vessels). There are also several other cells and proteins contributing to the blood-brain barrier complex; for example, processes called astrocytic end-feet extend from astrocytes to surround blood vessels and provide support to the endothelial cells of the blood-brain barrier.
What is the blood-brain barrier and what does it do?
The blood-brain barrier acts as an additional boundary between the circulating blood and the extracellular space of the brain. The barrier is highly selective, meaning it only allows certain substances to cross from the bloodstream into the brain. This functions to protect the brain from toxins, pathogens, and even circulating neurotransmitters (e.g., glutamate) that can be potentially damaging to neurons if their levels get too high. Only water, certain gases (e.g., oxygen), and other lipid-soluble substances can easily diffuse across the barrier (necessary substances like glucose can be actively transported across the blood-brain barrier with some effort).
It is thought that the central component of the functional anatomy of the blood-brain barrier involves tight junctions formed between endothelial cells, the cells that make up the interior surface of the blood vessels in the brain. In other blood vessels throughout the body, there are spaces between these endothelial cells; small blood-borne substances can pass through such spaces and into surrounding tissues. The endothelial cells that make up the blood-brain barrier, however, are fused tightly together, which restricts passive diffusion across the blood vessel lining.
Projections from astrocytes also extend to the walls of the blood vessels that are part of the blood-brain barrier and often completely surround those vessels. These projections, called astrocytic end-feet, appear to play critical roles in the formation of the blood-brain barrier. For example, they are thought to be involved with signaling that prompts endothelial cells to form the tight junctions necessary to create the blood-brain barrier. They also seem to have multiple functions involving the maintenance of the blood-brain barrier and possibly the transient opening of the barrier to allow important substances to cross in special circumstances.
While most blood vessels in the brain are ensconced in the blood-brain barrier, there are some regions that lack a blood-brain barrier, allowing substances to pass from the blood to the brain and vice versa more freely. For example, the circumventricular organs are a group of structures lacking a blood-brain barrier that are centered around the ventricles of the brain. It is thought blood vessels in the circumventricular organs are more permeable for a reason; for instance, the posterior pituitary gland needs to release hormones directly into the bloodstream and the subfornical organ is involved in cardiovascular regulation, which requires access to the circulatory system to monitor levels of hormones in the blood.
Although the blood-brain barrier is an important layer of protection between the peripheral blood circulation and the brain, in certain situations it can be problematic that access to the brain is so restrictive. For example, in the rare instance where there is an infection of the brain, the blood-brain barrier makes delivery of antimicrobial agents to the brain very difficult; it also impedes the passage of antibodies from the body to the brain. While in these cases the blood-brain barrier may be an obstacle to treatment, however, in general it provides an essential buffer between the circulating blood of the body and the brain.
Reference (in addition to linked text above):
Ballabh P, Braun A, & Nedergaard M (2004). The blood-brain barrier: an overview, structure, regulation, and clinical implications. Neurobiology of disease, 16 (1), 1-13.